Personal Science Week - 260430 HRV
My still-in-progress experiments with heart rate variability
Heart rate variability (HRV) is one of the best biometrics for understanding your body’s overall adaptability to stressors—food, sleep, exercise, pathogens, you name it.
Recently I’ve been testing HRV seriously to see what I can learn — and I’ve come away with a narrower, more useful theory than I started with.
On the morning of April 13, my resting heart rate (RHR) was 64—well above my baseline. That’s the kind of number that, on its own, just means something is off. Maybe I’m getting sick. Maybe I overtrained. Maybe I drank too much coffee.
But this time I had more data. I’d put on a Polar H10 chest strap (see PSWeek 260409) and run a 17-minute HRV recording through my HRV app. I got the autonomic signature of psychological stress, not illness, not overtraining.
Why was I stressed? Because I hadn’t started my taxes yet. (Personal scientists are not immune to procrastination.)
That morning is the cleanest example I have of why HRV is worth measuring. Resting heart rate alone could not have told me which kind of “off” I was in—and the right response is different for each.
What HRV is good for
After several weeks of exploring, my conclusion:
RHR is best for overall readiness scoring ; HRV helps figure out why something is off.
RHR is one of the easiest metrics to capture. Any activity wearable will give it to you (and you can even measure it the old fashioned way with a thumb on your wrist and a minute timer). HRV (heart rate variability) is much trickier to capture accurately—and most importantly—in a way that’s actionable. Spoiler alert: your Apple Watch or Oura measure of HRV are not particularly actionable, I’ve found.
The instructive cases in my data are when HRV and RHR disagree. When they agree, RHR is sufficient and HRV is redundant. When they disagree, HRV usually tells you something specific about which physiological state you’re in.
For daily decisions—did I recover, am I overreaching, should I train hard today—RHR captures something like 70–80% of what HRV tells you. It’s cheaper, less noisy, less artifact-prone. The 20–30% where HRV adds something is when it’s worth the extra trouble.
A quick HRV primer
If you’re new to HRV: it’s the tiny variation in milliseconds between consecutive heartbeats, and it’s a window into your autonomic nervous system—the involuntary side that regulates everything from digestion to stress response. Your heart’s pacemaker is designed to fire at a steady rhythm—about 100 bpm without input. The autonomic nervous system rides that pacemaker like a driver: the parasympathetic branch acts as a brake (slowing things down at rest), the sympathetic branch as an accelerator. HRV is a measure of how actively that driver is steering—how quickly your body shifts between the two.
Higher variability generally means a more responsive parasympathetic (”rest-and-digest”) branch; lower variability means the sympathetic (”fight-or-flight”) branch is dominating.
Apple Watch will report an HRV number (SDNN, sampled overnight), but it samples sporadically and the absolute values are noisy. Oura is better, but it’s still only every 5 minutes. For serious and actionable metrics, you’ll want a chest strap.
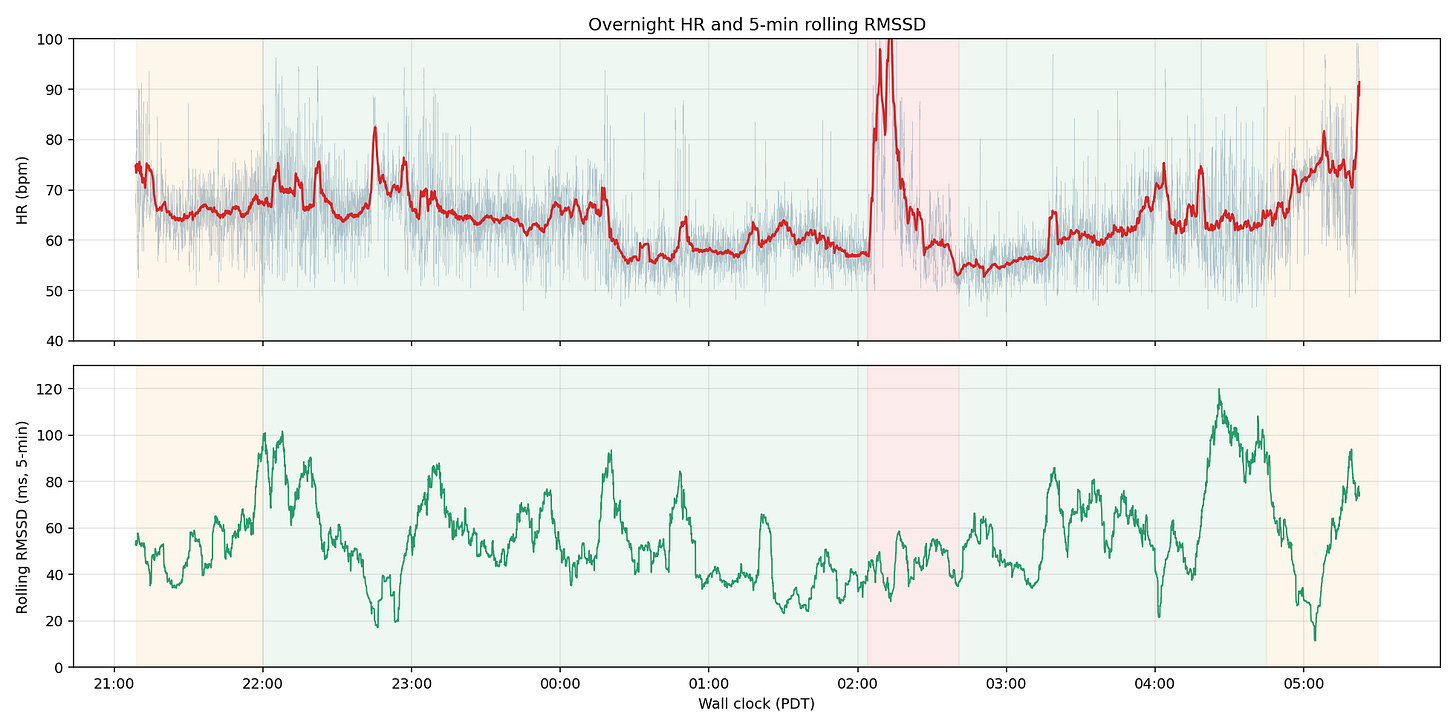
1. Am I getting sick? (24–48 hours of warning)
This is the case that justifies the overhead for most people, including me.
A controlled influenza H3N2 challenge study (Temple et al., 2023) inoculated 20 healthy adults with flu virus and monitored HRV, heart rate, and activity via a wearable for 7 days before and 10 days after. Their anomaly-detection model correctly flagged 16 of 17 infected participants an average of 23 hours before symptom onset—and 58 hours post-inoculation, well inside the window where rest and hydration actually change the trajectory.
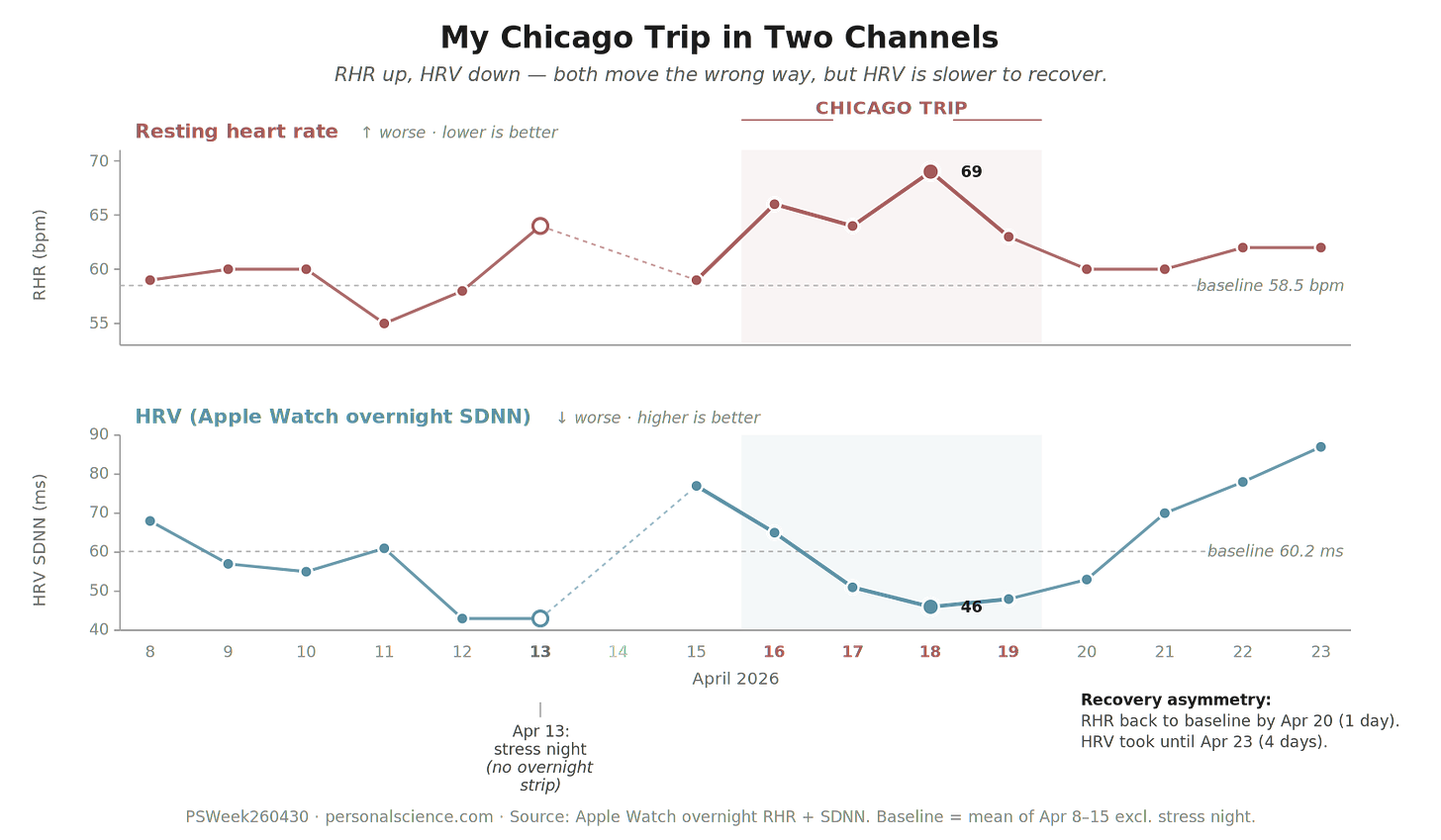
My own data has a blurrier version of this. In March I caught a rhinovirus, and my HRV dropped before I consciously registered anything was off (see PSWeek260402). But I had a similar drop during my Chicago trip earlier this month—cross-country flight, late-night wedding reception (congrats Leah and Keegan!), a glass of wine here and there. Both recovered, but HRV took about four days to return to baseline while RHR was back within two. Nothing viral; just a clean "something is off" signal — visible in both channels.
The practical version: if Watch HRV drops more than 1.5 SD below my baseline for two consecutive nights and RHR is up 5+ bpm, I flag it as “possible incubation” and adjust the day accordingly—hydrate, cancel the hard workout, reschedule travel if I can. Sometimes it’s nothing. Sometimes it’s something.
2. Is this stress, or fatigue, or something else?
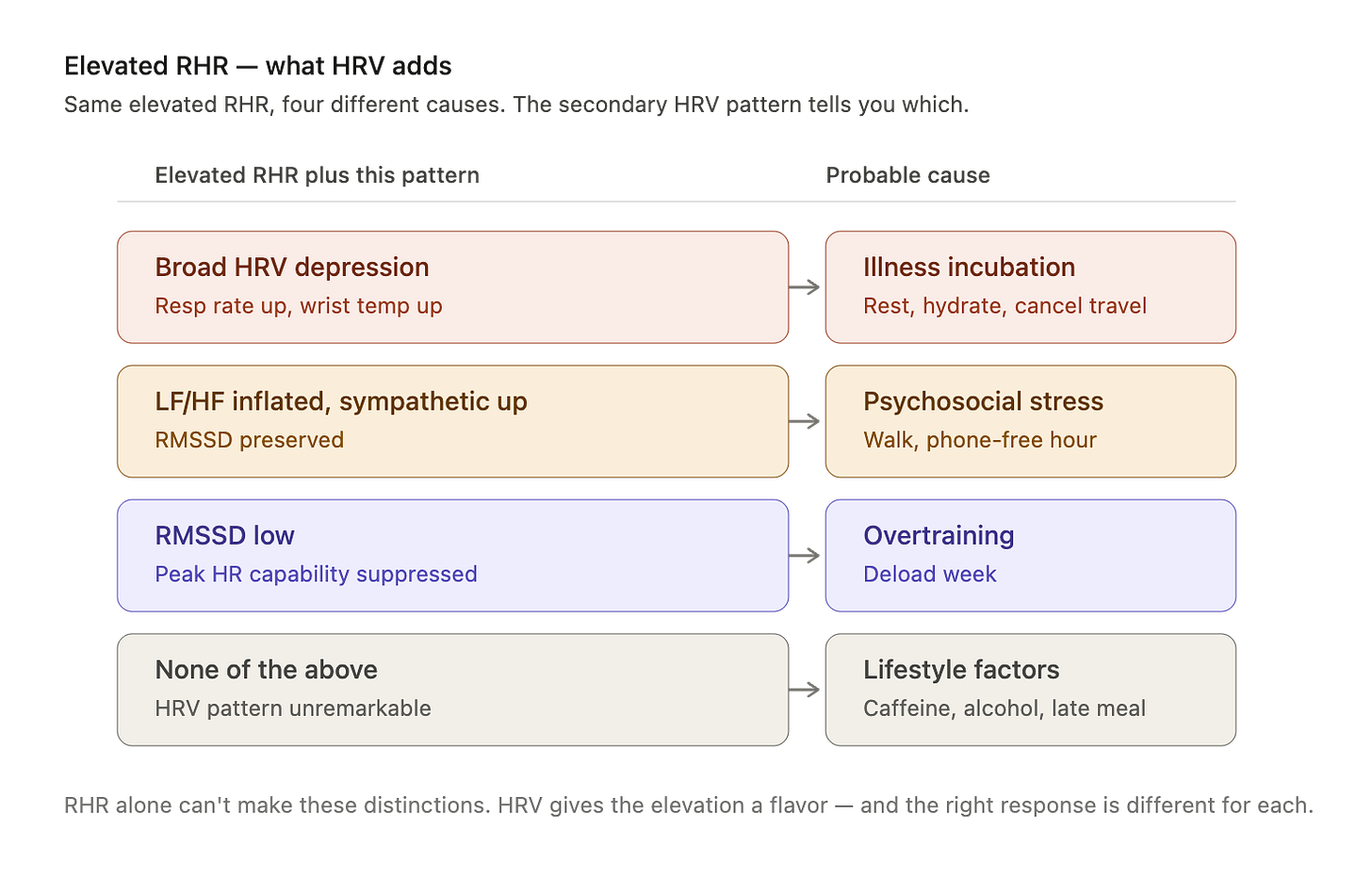
Back to the April 13 morning. Elevated RHR has a half-dozen possible causes, and HRV gives the elevation a flavor. Here’s the rough differential that seems to work:
RHR alone can’t make these distinctions. HRV can. What you do about each is different—the stress case calls for a walk and a phone-free hour, the overtraining case calls for a deload week, the illness case calls for bed. Getting the category right matters.
What HRV doesn’t do
Being honest about what you’re not getting is half of personal science.
It doesn’t predict sleep quality. My best night this month and my worst night had similar morning HRV. What predicts how rested I feel is RHR + N3 duration + what stage I wake up in. Not HRV. (See PSWeek260416 on the protein-sleep relationship.)
It’s not a fitness benchmark. Resting HRV correlates only weakly with VO2max cross-sectionally. Useful for tracking your own change over months; useless for comparing yourself to anyone else.
It’s not a mortality oracle. Yes, population-level HRV correlates with cardiovascular outcomes. The effect sizes are small enough that no single personal decision turns on it.
My current HRV toolkit
Here’s what I’m using now:
Free and good enough: Apple Watch overnight RHR and its HRV measure (SDNN). Catches the big perturbations—Chicago-trip-level stuff, illness incubation, holiday weekends. Fine for most people. I wear my Watch to bed anyway, so this is essentially zero marginal effort.
Cheap and much better: Polar H10 chest strap (~$90) plus the free Kubios HRV app. Two minutes of setup each morning. ECG-grade beat detection. Every frequency-domain metric you’d want—and this is what enabled the April 13 stress-vs-illness call.
If you want to go deeper: pair the H10 with the HRV Logger app by Marco Altini ($15). It exports raw RR intervals to SQLite and CSV, so you can run your own DFA α1, Poincaré, and time-domain analyses. I export mine into a longitudinal log and have Claude pattern-match across mornings.
I don’t use an Oura ring. At $400 plus a monthly subscription, it’s expensive for something whose main job—telling you how you slept—you mostly already know by how you feel. The Apple Watch + H10 combo gives me more data for less money.
For more information about personal HRV monitoring, the best source is Marco Altini’s HRV4Training blog. The creator of HRV Logger writes clearly and honestly about what HRV can and can’t do, mostly for high performance-seeking athletes but also for the rest of us.
Personal Science Weekly Readings
Speaking of low cost new ways to quantify yourself:
Is it really possible to use an off-the-shelf iPhone as an ultrasound camera? Apparently, yes—researchers have built an app that turns the phone’s existing hardware into a fetal heart monitor.
Seth Howe is a basically normal guy who sequenced his DNA at home using a $3,200 MinION Mk1D sequencer and about $1,100 of reagents. He also needed access to a centrifuge, heat block, and pipettes—items found in any biology lab. (Easier alternatives: a 30x sequence from sequencing.com for ~$400, or The Odin’s $599 deal if you want to keep your raw data private.)
A 2023 study concluded that more than three-quarters of a million Americans are permanently disabled or die each year as the result of a misdiagnosis—about 5% of Americans experience a wrong diagnosis annually. A useful reminder of why personal scientists treat clinical conclusions with the same skepticism we apply to supplements.
About Personal Science
Personal scientists approach wearable data the way we approach everything: with open-minded skepticism and a willingness to experiment. We don’t assume the marketing claims are right, and we don’t assume they’re wrong. We track, we compare, we update our models. Nullius in verba.
We publish every Thursday. If you’ve found uses for HRV data that RHR doesn’t give you, let us know.